Clinical Urology
Clinical urology refers to the branch of medicine that focuses on the diagnosis, treatment, and management of urological conditions in patients. Urology is a specialty that deals with the urinary tract system (including kidneys, bladder, ureters, and urethra) and the male reproductive system (including the prostate, testes, and penis).
Clinical urologists evaluate patients with various urological disorders such as urinary tract infections, kidney stones, bladder problems, prostate conditions (like benign prostatic hyperplasia or prostate cancer), urinary incontinence, erectile dysfunction, and infertility. They employ a range of diagnostic techniques, including physical examination, imaging studies, laboratory tests, and may perform surgical or non-surgical interventions to treat urological conditions and improve patient outcomes.
Clinical Urology mainly includes:
- Conservative or OPD Management of Urological Disorders – Conservative or outpatient department (OPD) management of urological disorders involves non-surgical or non-invasive approaches to diagnose, treat, and manage urological conditions. It typically includes the following aspects:
- Initial evaluation: Patients undergo a thorough medical history assessment, physical examination, and may be recommended diagnostic tests such as urine analysis, imaging studies, or blood tests to aid in diagnosis.
- Medications: Pharmacological interventions, such as antibiotics for urinary tract infections, alpha-blockers for benign prostatic hyperplasia (BPH), or medications for erectile dysfunction, may be prescribed to manage urological conditions.
- Lifestyle modifications: Patients are advised on adopting lifestyle changes that can alleviate symptoms or improve overall urological health. This may involve dietary modifications, increasing fluid intake, bladder training, or pelvic floor exercises.
- Behavioral therapy: Techniques such as bladder retraining or biofeedback therapy can be used to manage urinary incontinence or overactive bladder symptoms.
- Counseling and education: Patients are provided with information about their condition, its management, and potential complications. They may receive counseling on sexual health, contraception, or fertility preservation.
- Follow-up and monitoring: Regular follow-up visits are scheduled to assess treatment effectiveness, monitor progress, and make adjustments as necessary.
Conservative or OPD management is often the first-line approach for many urological disorders, focusing on non-invasive interventions and patient education to improve symptoms and quality of life. If conservative management fails or the condition worsens, further interventions such as surgery may be considered. The specific management plan is tailored to the individual patient’s needs and the nature of their urological disorder.
- Urodynamic Study – Urodynamic study is a diagnostic test used to evaluate the function and behavior of the lower urinary tract, including the bladder, urethra, and associated muscles. It involves a series of measurements and assessments to understand how the urinary system is functioning. Here are the key components of a urodynamic study:
- Uroflowmetry: This measures the rate and volume of urine flow during voiding. The patient urinates into a special device that records the flow rate.
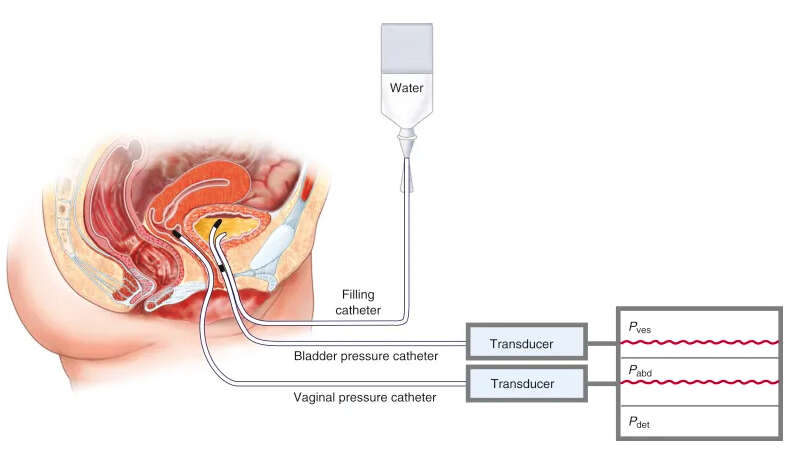
- Cystometry: This assesses the bladder’s capacity, pressure, and sensation. A catheter is inserted into the bladder, and the bladder is filled with sterile fluid. The pressure inside the bladder is measured as it fills and empties, providing information about bladder function.
- Pressure Flow Study: It evaluates the pressure generated by the bladder during urination. Simultaneous measurement of bladder pressure and flow rate helps diagnose conditions such as bladder outlet obstruction.
- Electromyography (EMG): This measures the electrical activity of the muscles surrounding the bladder and urethra. It helps assess muscle coordination and can identify abnormal muscle contractions.
- Urethral Pressure Profile: This measures the pressure inside the urethra at rest and during stress or coughing. It helps identify urethral obstruction or weakness.
- Leak Point Pressure Measurement: It determines the pressure at which urine leakage occurs during increased abdominal pressure. This can assist in diagnosing stress urinary incontinence.
Urodynamic studies provide valuable information to diagnose conditions such as urinary incontinence, overactive bladder, neurogenic bladder dysfunction, and bladder outlet obstruction. The results help guide treatment decisions and management strategies for urological disorders. The test is typically conducted by a urologist or specialized urodynamic technician in a hospital or clinic setting.
- Uroflowmetry – Uroflowmetry is a non-invasive diagnostic test that measures the rate and volume of urine flow during voiding. It provides information about the function and efficiency of the lower urinary tract, specifically the bladder and urethra.
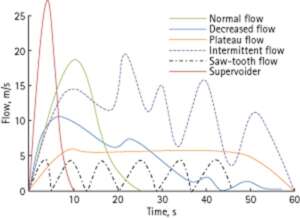 Uroflowmetry is commonly used to evaluate urinary symptoms such as weak urine flow, frequent urination, or incomplete bladder emptying. It can help in the diagnosis of conditions like urinary obstruction, benign prostatic hyperplasia (BPH), urethral strictures, or bladder dysfunction. Uroflowmetry results, in combination with other diagnostic tests, can assist doctors in determining appropriate treatment options and monitoring the effectiveness of interventions for urological conditions.
Uroflowmetry is commonly used to evaluate urinary symptoms such as weak urine flow, frequent urination, or incomplete bladder emptying. It can help in the diagnosis of conditions like urinary obstruction, benign prostatic hyperplasia (BPH), urethral strictures, or bladder dysfunction. Uroflowmetry results, in combination with other diagnostic tests, can assist doctors in determining appropriate treatment options and monitoring the effectiveness of interventions for urological conditions.